
The Los Angeles headquarters of onefinestay, a high-end Airbnb competitor where Megan Peri worked until June of last year, was open plan. The only rooms with doors were the bathrooms, the conference rooms, and the closet where the company kept its server towers. Peri recalls the conference rooms were “coveted spaces where you had to get on the calendar weeks in advance,” and the bathroom was a non-starter, so after the birth of her first child in 2016, she chose the closet to pump. It didn’t lock, so she taped a note to the door and wrapped a power cord around the handle. “The server closet didn’t actually have a wall that went all the way to the ceiling, so people could hear the machine,” she tells me.
Although she found it awkward, Peri didn’t press for a more private place. “It’s already challenging enough to be pregnant or a new mother in the workforce,” she explains. “You don’t want to be taking more time and—I don’t know, compromising your work ethic, or whatever it might be. So, you just make do.”
Peri is one of many white-collar American women who return to work after giving birth only to find that pumping is one of the most challenging aspects of the transition—whether because of lack of facilities, byzantine access procedures, or a workplace culture that scrutinizes new parents and discourages taking breaks. Over email, Peri reiterated that she knows her former employer was not “malicious or neglectful, I just think they thought it was no big deal…And I made it work.” She’s also grateful for the company’s policies on flexible scheduling, maternity leave—she received three months, paid—and remote work, which Peri regularly used. But, when she was in the office and had to pump, she says, “There was just never a good spot to do it. Ever.”
(A onefinestay spokesperson pointed out that the company’s New York office does have a lactation room, and added, “Our new Los Angeles office, where we are moving shortly, will have a designated pumping room. It is very important to give new mothers a safe and completely private space to pump as often as they wish.”)
While tech as an industry is far from unique in paying sometimes spotty attention to the needs of nursing workers, the fact that the sector is known for lavish perks—the gourmet cafeterias serving free meals, pet-friendly offices, on-site massage therapists, nap pods, workout classes, and even game rooms—can make a lack of planning for lactation rankle.
The co-working giant WeWork, which offers such non-essentials as ping pong tables, meditation rooms, and complimentary craft beer, was criticized by some tenants in 2015 for not having lactation rooms. The company’s FAQ page includes information on bringing your dog to work and reserving a conference room in Colombia, but makes no mention of lactation. A WeWork spokesperson declined to comment when asked how many of the company’s U.S. locations currently offer lactation rooms. Meanwhile, female-friendly co-working spaces such as the Wing and the Riveter openly advertise lactation rooms among their amenities.
If finding an appropriate space to pump can be difficult for a worker based in one location, it becomes even more so when routines (the importance of which I’ll get to soon) are interrupted. I heard from women who had to negotiate pumping at off-site meetings or client premises, and who spoke of conferences where the temporary lactation room had only one outlet (meaning space for only one pump) and a long line of mothers waiting to use it. In June, at Apple’s famous Worldwide Developers Conference where the company unveils its new technologies and products, Arianna Huffington posted publicly about an incident where Yardley Ip Pohl, the Chief Product Officer at Huffington’s company Thrive Global, had to pump in a car outside the venue after two Apple conference staffers told Pohl there was no lactation room. That later turned out to be incorrect—Apple had set aside a room for pumping—but Pohl had already improvised. Huffington shared a photo of Pohl pumping in the vehicle. (Pohl, via a Thrive Global spokesperson, declined to comment directly, but confirmed the account of these events.)
The tech world also offers potential solutions. There’s the company Mamava, which manufactures freestanding private “lactation pods” in various sizes for workplaces and public spaces like airports, stadiums, and malls. For mothers whose jobs require domestic travel, the start-up Milk Stork offers prepaid overnight shipping and pharmaceutical-grade coolers to send breast milk home from the road. (Shipping for a 34-oz cooler costs $139. The company also has corporate accounts, so companies can offer Milk Stork’s services as a perk.) Peanut, a social networking app for mothers, provides a release valve for women to swap stories. Among its 300,000 users, discussions about pumping, breastfeeding, and returning to work come up frequently. “I think that’s testament to the fact that we needed a place to have these types of conversations, and it was long overdue,” says Peanut CEO and co-founder Michelle Kennedy.
But from conversations with women around the country who have recently negotiated pumping in their workplaces, it seems that plenty of companies aren’t aware of—or don’t understand the value in—the steps that can make workplace lactation easier for new mothers.

The American Academy of Pediatrics (AAP) have recommended that babies be breastfed for at least 12 months, and that they consume breast milk exclusively for the first six months, which is around the age when infants can begin to eat solid food (the World Health Organization also recommends that babies be breastfed for the first six months). Breast milk, a nutritionally balanced meal that provides essential nutrients as well as antibodies to protect newborns against infectious disease, has been shown to lower rates of childhood obesity (childhood obesity can lead to adult obesity, insulin resistance, depression, anxiety, and poor learning), and even sudden infant death syndrome. Some studies have suggested that breastfeeding may also lead to lower rates of asthma. For mothers, breastfeeding leads to a lower risk of type 2 diabetes, certain types of breast cancer, and ovarian cancer.
To feed a newborn and establish a milk supply, a mother needs to express milk as often as every 2-3 hours, and although that frequency eases as her baby grows, most women still need to pump at least twice in an average work day. Skipping a session is not only physically uncomfortable, it carries the risk of complications like blocked ducts or mastitis. In the short-term, you might leak through your shirt, and in the long-term, skipping or delaying pumping signals the body to start making less milk, imperiling your supply. Unlike parental leave or flexible scheduling, which to some extent affect all working parents, breastfeeding is a labor of parenting that can only be performed by mothers. And so it’s mothers who are left to negotiate the workplace issues that arise from it.
Four out of five American mothers start out breastfeeding, according to the Centers for Disease Control and Prevention’s most recent figures, but their desire to breastfeed runs up against a number of barriers. Only about one in five mothers actually manages to exclusively breastfeed for the first six months, as the WHO and the AAP recommend.
Maternity leave—or the lack of it—is the first and biggest hurdle that women who wish to breastfeed face. The U.S. is the only industrialized country without paid maternity leave, so American women work much later into their pregnancies and return to work sooner after giving birth than many women elsewhere. One study found that almost a quarter of U.S. women are back at work within two weeks of giving birth. Black mothers on average also return to work sooner than white mothers. Only 16 percent of full-time workers have access to paid parental leave as a benefit, so the most common American “maternity leave” is actually a kind of franken-leave mothers create out of sick days, vacation days, disability, and unpaid family medical leave.
Returning to work early can disrupt a nascent breastfeeding relationship, but many American women can’t take an extended unpaid leave because their families rely on their income. Since the mid-1980s, working motherhood has been the norm, not the exception. According to the Bureau of Labor Statistics, 58 percent of mothers of infants under 12 months are in the workforce. Mothers who work outside the home increasingly do so not as some kind of add-on, but to support their families. More than 40 percent of mothers in the U.S. are family breadwinners. Among black mothers, the figure is more than 70 percent.
“On one hand, as a society, we keep saying how important, how imperative it is for infant health and for women to be breastfeeding, but then we do completely the opposite when it’s time for women to go back to work,” says Dr. Lauren Dinour, an assistant professor in the Nutrition and Food Studies department at Montclair State University in New Jersey, who has published extensively on breastfeeding and pumping in the U.S. “We don’t give them adequate time at home with their infant necessarily to even establish a healthy breastfeeding relationship. That takes at least three or four weeks, but many women don’t get any kind of maternity leave. Many women work in workplaces where there is no such thing as break time, or they’re paid by the hour and they don’t want to give up an hour in their day to breastfeed, because that’s an hour less that they’re going to get paid—and oftentimes money is extremely important when you have a newborn, especially if you’re the sole source of income.”
Dinour is frustrated by how breastfeeding is often framed as a matter of women’s individual choices, rather than of environmental supports and policies that influence behavior. That framing, Dinour says, can send the message that creating the circumstances for successful breastfeeding is a woman’s responsibility alone. “It’s not just a choice of ‘Yes’ or ‘No’ to breastfeeding,” she says. “It’s a choice of, ‘Can I overcome these barriers that are in place for me?’ And for many women, the answer is no.”

Traveling for work poses daunting challenges for mothers of infants, especially breastfeeding mothers. “You have to store up quite a lot of ounces before you leave,” says Nancy Rosenbloom, the sales director at fashion brand Rachel Comey, which is headquartered in New York City. Rosenbloom makes four week-long trips to Paris each year. When she was nursing, it took her several weeks of stockpiling to prepare for each trip—pumping an extra 4 or so ounces every session. “That was insanity,” she says now. “It was just too much.”
Peri traveled often for work while she was pumping. “I remember going to a conference in Vegas, staying in a five-star hotel that had one of those sensored fridges where you can’t touch anything, because if you touch it, it charges you.” When she called the front desk to ask to clear the fridge so she could use it to store milk, they told her there was a fee. “I was like, ‘Well, I need it for pumping.’ And they were like, ‘Well, we don’t care.’” Finally, Peri called back and said, ‘Look, I’m in [the travel] industry, and you have to bring me a fridge or you have to clear this one, because I have to pump.” The hotel complied.
And then there’s air travel. The Transportation Security Administration considers breast pumps medical devices, and both breast milk and formula are exempt from the carry-on liquids limits. If they’ve gone slushy, the TSA can confiscate the ice packs used to keep breast milk cold. “So you’re dependent on the benevolent Starbucks worker who will [give you] ice, even though they’re not supposed to,” says one frequent flying woman. In addition, TSA agents may at their discretion open and test containers of breast milk, a process that can be time-consuming, not to mention unnerving to mothers who are constantly sterilizing bottles and pump parts to avoid contamination. I talked to moms who have had TSA agents swab or dip litmus strips into every bag or bottle of breast milk they were carrying. Others said agents asked them, “Where’s the baby?” (A baby’s presence is not required to carry breast milk or a pump on a plane.)
A 2014 study looked at access to lactation rooms at 100 U.S. airports and found that while almost two-thirds described themselves as being “breastfeeding friendly” and 37 reported having lactation rooms, only eight actually had a space, other than a bathroom, with an electrical outlet, table, and chair, which the study authors considered the minimum requirements for a lactation room. Most airports considered a family restroom a “lactation room.” Illinois Democratic Senator Tammy Duckworth—who recently gave birth to her second daughter—has introduced a bill that would let airports use existing federal funds to build lactation rooms. In an op-ed for Cosmopolitan, Senator Duckworth wrote that her experiences of air travel as a new mother partly motivated her to draft the legislation.
On longer flights, a nursing traveler may need to pump on the plane. “It’s really weird to pump while you’re sitting next to a stranger,” says Peri. “And then if you go in the bathroom, the bathroom of an airplane is one of the most unsanitary places in the world.” Peri estimates she had to throw away 30-50 percent of the milk she pumped while traveling because of questionable sanitation or refrigeration.
When she was on a business trip and her son was about four months old, Peri realized at the airport she’d forgotten a crucial part for her pump. “I’m sitting there literally about to get sick from being engorged, which is a terrible word,” she recalls. Peri knew it was possible to express milk manually, but she had never done it. So she ducked into a family rest room and started searching on her phone for a how-to video.
“I found YouTube videos of self-expression,” Peri says. “But—they were perverted. It’s a fetish thing. And I cannot find a proper video to explain it to me, because all I keep getting are these fetish videos.” Painstakingly, Peri eventually managed to express milk by hand, but the whole experience was miserable, her fear of mastitis and her anger at the algorithms surfacing pornography masquerading as women’s health colliding in an airport bathroom.
(When we contacted YouTube with examples of a dozen breastfeeding-related videos that seemed intended to titillate, YouTube agreed that they violated the company’s policy. The videos were promptly taken down.)
“Three months later, I was in Vancouver for work when I found I was missing a part, and I just said, ‘Screw it,’” says Peri. “That’s when I gave up. I was like, this is just not going to work. We switched to formula—and it was fine.”

Pumping in the workplace has been protected under federal law since the 2010 passage of the Affordable Care Act. Under the ACA, companies must provide their nursing hourly employees with “reasonable” break time to express milk and a private place in which to do it. The breaks do not have to be paid, and the space does not have to be a dedicated lactation room—but it must be “shielded from view and free from intrusion by coworkers and the public,” and it cannot be a bathroom. Salaried employees, and all other workers who are exempt from overtime requirements under the Fair Labor Standards Act, are not covered. In a separate provision of the ACA that came into effect in 2012, the law also required health insurance plans to cover breastfeeding support services and breast pumps, without additional charges. (Basic pumps are also covered by Medicaid.)
The workplace pumping provision wasn’t in the original draft of the bill, and its inclusion came about in large part because of Oregon Senator Jeff Merkley. As a freshman on the influential Committee on Health, Education, Labor and Pensions, the Democrat saw an opportunity to propose it as an amendment during the committee’s contentious debate over the ACA. Merkley had workshopped the idea of creating workplace support for pumping within his own party, and with New York congresswoman Carolyn Maloney, who had been working on the issue for 10 years in the House, without success. But he didn’t tell anyone across the aisle, because he didn’t want to give the business community a chance to lobby against it. “I hoped that [my] argument would win the day,” says Merkley, on the phone from his office.
To Merkley’s great surprise, his measure found support from an unlikely source: Oklahoma Republican Senator, Tom Coburn. An obstetrician prior to entering the Senate, Coburn opposed the ACA, and in committee he “was pretty much eviscerating one Democratic amendment after another,” recalls Merkley. But when Merkley brought up pumping, Coburn spoke passionately on the advantages of breastfeeding for mothers and babies, and the need to encourage it. Merkley’s amendment passed unanimously out of committee and went on to become law.
Merkley wrote his amendment to apply to hourly, not salaried, workers. In retrospect, he regrets the exclusion. “I wish we had done it for salaried workers as well,” he says. Merkley drafted it with the salaried workers exemption because he thought it had a better chance of passing, and because low-wage hourly workers needed the law’s protections more. “The sense was the salaried world has a lot of flexibility currently, compared to the waged world, so the biggest need was in the waged world,” he explains.
There’s an obvious logic behind workplace pumping laws. Most American women work, including those who are mothers of infants. Because breastfeeding is a round-the-clock commitment, employers can play a critical role in supporting their employees’ nursing. More than eight years have passed since the ACA and its workplace pumping provision became law, and many employers aren’t complying. One study found only 40 percent of working mothers of infants have access to both a private place to express breast milk and break time in which to do it. Among black and Hispanic mothers, it’s 14 percent.
It’s hard to imagine stronger pumping laws getting any White House support under President Trump. Trump once called an opposing lawyer “disgusting” for asking to take a pre-scheduled pumping break during a 2011 deposition. Just last week, the U.S. delegation to the United Nations surprised allies by demanding the removal of language promoting breastfeeding from a resolution, and even threatened Ecuador and other countries with sanctions if they did not withdraw their support. The resolution only passed when Russia threw its weight behind it.
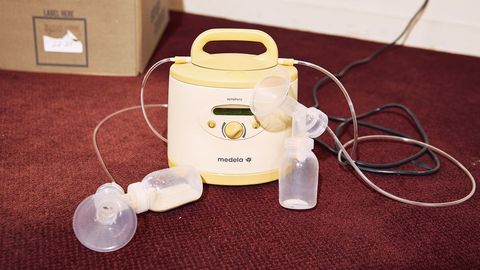
While it remains to be seen whether the federal laws governing workplace lactation will ever be expanded to cover more workers, scholars and others have begun to assess the impacts of the ACA. It seems to have done a lot for breast pump manufacturers: During the two years after breast pumps were covered by insurance, sales at Medela, the leading pump maker, rose by 34 percent. But the law’s impact on breastfeeding is a little harder to parse. One of the most comprehensive studies yet of the ACA’s impact on breastfeeding behavior was published this March. It found that the law’s impacts were fairly modest, only slightly increasing the likelihood of breastfeeding initiation in the U.S.—out of around 4 million births in 2014, the researchers concluded the law change led to about an additional 47,000 infants receiving at least some breast milk. (The biggest impact was on black, less educated, and unmarried mothers, all of whom historically have lower rates of breastfeeding.) The study also found that the ACA increased the average duration of breastfeeding. The amount of that increase? About two weeks.

As Jeff Merkley’s experience with Tom Coburn attests, frontline health care workers are usually well-versed in the benefits of breastfeeding. But even as doctors and nurses promote breastfeeding to patients, their own working conditions sometimes make pumping difficult.
Sarah, a registered nurse at Northside Hospital in Atlanta who spoke on condition of anonymity, said she is currently struggling to pump at work. She and her colleagues, several of whom are also pumping, work 12-hour shifts. Sarah gets to work early so that the last thing she does before clocking in is pump; that way she can go as long as possible before taking a break. When her shift begins at 7 a.m., that means rising at 3:45 a.m.
“Typically, the way our patient flow goes, I probably won’t get another opportunity to pump until about 9 or 10 a.m.,” she says. “From there, it varies. A lot of days, we don’t even have the staffing to relieve people for lunch. I have to tread lightly asking for a pump break when most people aren’t even getting lunch breaks.”
Although she finds waiting more than three hours between pumping sessions uncomfortable, she sometimes has to go more than four. Still, Sarah says, her coworkers “grumble” about her and her colleagues’ lactation breaks. “There’s been a lot of talking about how unfair it is,” she explains. “They think we only need to be off the floor 10 minutes. When, in reality, getting everything set up, pumping, breaking it down, cleaning it up, and getting back to the floor, it may take 30 minutes.” The nurse says she personally isn’t fazed by her coworkers’ reactions—“I will basically tell people where to stick it”—but she is frustrated by the pressure that the scheduling and staffing levels put on all of them.

The nurse has hesitated to raise these issues with HR—the griping coworkers, the lack of privacy in the locker room—because she knows, legally, the hospital could start requiring her and her colleagues to clock out for pump breaks.
When asked about its policies on lactation, a hospital spokesperson said it is Northside’s policy to pay employees during lactation breaks, in addition to two other paid breaks per shift. The spokesperson said when workers return from maternity leave, supervisors should coordinate with nursing mothers so they can access private offices with locking doors to use as lactation rooms. “Employees should never feel guilty about taking lactation breaks,” the spokesperson said. “If issues arise, we address them with appropriate measures that support the new moms and better inform the staff of lactation protocols.”

Of the women interviewed for this piece who ran into problems pumping at work, none went to their bosses or to HR. That’s not surprising, according to Kristin Rowe-Finkbeiner, the CEO of the activist group MomsRising, which focuses on issues facing mothers and families. Rowe-Finkbeiner argues the reality of employment discrimination against mothers often deters women from speaking up. “When we’re talking about public policies relating to breaks for pumping and safe, private spaces for pumping, we’re coming at this in a culture and in a climate where moms are judged more harshly, moms are paid less, and advanced less often.” Women, she says, don’t want to be seen as complaining for fear of retribution.

Because White’s son was a preemie, access to breast milk was critical because of its immune antibodies. But he also had trouble feeding—the suckling reflex is one of the last characteristics to develop in utero—and White had difficulties generating milk. “I sort of missed that initial time [at home] that would have helped me establish a supply,” she says on the phone from Kansas. Neither the building where White taught nor the building where she had her office and most of her classes had a lactation room. When White asked an administrator for a place to pump, she suggested White use a faculty member’s office, or go to a restroom. White didn’t feel comfortable asking any of her professors for such a favor, and as for the restrooms, they were not terribly clean and often filled with undergrads. “I mean, I like having a casual relationship with my students, but that’s crossing a line,” says White. “I couldn’t do it.”
When another student in White’s program became pregnant and successfully pressed for leave, albeit unpaid, White says she realized she could have demanded more from the university. But she “didn’t want to be seen as somebody who was ripping off the system or taking more than my fair share.” At the time, White was also under consideration for a new teaching assistantship. “I didn’t want to be seen as being too needy, or being unable to work within whatever was available to me,” she says. “I wanted to be seen as flexible, and able to power through things, and get things done.”
Although it had been her goal to breastfeed her son exclusively for at least six months, White had to begin supplementing her milk with formula, which her son didn’t tolerate well because of not-yet-diagnosed allergies. “Every time I would see him wince in pain because his digestive system just wasn’t handling the formula well, it was just a guilt trip,” White recalls. After four months of breastfeeding and supplementing with formula, White’s milk supply still wasn’t robust. Her pediatrician told her it was okay to stop pumping. “It was a tremendous relief for me, but it didn’t help my son,” says White. “He would have been so much better if he’d had access to breast milk.”
When asked about White’s account, a spokesperson for the University of Iowa said the university is committed to supporting nursing parents on campus. “The University of Iowa works to provide an environment and culture where employees becoming new parents are treated fairly during pregnancy, upon their return to work, and beyond to allow them the ability to be successful in their professional lives and to provide a supportive work/life balance.” Since 2010, all new campus buildings have been designed with lactation rooms, and the Iowa campus now has more than 60 such rooms, although according to public listings, many of those are open limited hours or have other access restrictions. The University of Iowa said it has no current plans to add lactation rooms in the older buildings where White worked.
Last year, MomsRising launched a viral campaign called #IPumpedHere where working mothers posted pictures of places they pumped out of necessity, including supply closets, bathrooms, and their own cars. “We really wanted to make public what is often a private struggle,” says Rowe-Finkbeiner. “When this many people are struggling with the same thing at the same time, we don’t have an epidemic of personal failures. We have a structural issue that we can and must solve together.”

Of the women interviewed who had more positive experiences with pumping at work, most worked for smaller companies—under 100 employees—and several worked in female-dominated industries or under a female C.E.O. Nancy Rosenbloom, the Rachel Comey sales director, says motherhood is normalized in her workplace in a way that is welcome. “I would be in showroom appointments, and a buyer would plug in her pump in the corner and start pumping under the table as she’s writing an order, or another new mom would bring her baby and hop over to the corner in between deliveries and breastfeed,” she says. “There was no judgment.” Rosenbloom joined the company six months after she gave birth to her first child, after deciding not to return to her previous job following an unpaid maternity leave. Pumping came up at the interview, and Comey, the company founder, encouraged Rosenbloom to take whatever pump breaks she needed.

The open plan office meant Rosenbloom most often pumped in a bathroom. “But, to be honest, it didn’t really bother me,” she says. The bathroom had a shelf and a chair. She sipped water and, like virtually all the women I interviewed, brought her laptop so she could work through her breaks. (Several even took Skype or conference calls while pumping, their microphones muted to hide the droning of the machine.)
Like Rosenbloom, Sandi D’Avella works in the fashion industry in New York City, as the sales director of women’s footwear and accessories for the label Rag & Bone. “It’s very hard to transition back as a working mother,” says D’Avella, who has had two children during her time at Rag & Bone, both times pumping in the office following paid maternity leave of 11 weeks. She rented a hospital-grade Medela pump from a pharmacy for around $75 a month, which was quieter and faster than other pumps. She also invested in a slower, battery-powered pump, for traveling or whenever she didn’t want to be tethered to an outlet.
“With my first child, I think I was one of very few people [at the company] that had had a baby and needed to pump,” D’Avella recalls. “They created a little room. It was kind of a dark, scary little space in the corner, but it was fine. It did the job. Then, for my son, a lot more people had had babies. There was a schedule, we had a group email so we all could let each other know when we were in the pump room. There was a fridge. It was just a little bit more evolved than the first time around.”
In an environment with the proper workplace support, the discomfort of pumping can be mitigated with planning. Money helps, too. Women who are financially stable can buy a better breast pump than the models typically covered by insurance (like the wearable breast pump, Willow, which retails for $479), or even buy a second pump so they can leave one at work to minimize the hassle of commuting with a pump and the risk of leaving a part behind. But if there’s one thing that underlies so many of these interviews, it is the feeling of being valued.
Yes we are hosting a ton of editors as we launch our new product @yourfinery . Yes I am in a back room pumping as they talk outside. Yes this sucks. But YES this is why it’s awesome to be a part of a female founded, female-run startup.
A post shared by Brooklyn Decker (@brooklyndecker) on
Women who have to pump in a less-than-ideal space can feel fine about that, if they otherwise have the sense that their company cares about them and has thought about their needs. It also helps if it’s clear that the company is doing its best with the space and resources available—something actress Brooklyn Decker acknowledged at the launch of her new app, Finery, in April. “Yes I am in a back room pumping as they talk outside,” she captioned an Instagram image. “Yes this sucks. But YES this is why it’s awesome to be a part of a female founded, female-run startup.” On the flip-side, women who have access to a dedicated lactation room can feel demeaned if it’s poorly designed or they are scrutinized for using it, or if they otherwise see their employer treating maternity as an exceptional event.
Working women and female family breadwinners have been a reality in the U.S. for a long time. Wage gaps and glass ceilings aside, we’ve let women into almost all echelons of the working world, but, in some ways, we are still treating the male experience of work as the standard, and working women and their needs as the variant. “The truth of the matter is that our economy has changed, and our workplaces have changed, but we haven’t updated our public policies to reflect that,” says MomsRising CEO Rowe-Finkbeiner. “We need the whole gamut, from workplace policies to culture changes.”
There are a number of steps employers can take to support employees who want to pump, and not all of them are costly. Last year, Dinour, the academic who studies breastfeeding, co-authored a systematic review of studies of workplace breastfeeding accommodations in the U.S. and abroad and analyzed the effects of various interventions on breastfeeding behavior. The measures that have the biggest impacts are straightforward: providing a place to pump and allowing workers breaks to do it. One study found that women with access to both were 2.3 times more likely to exclusively breastfeed at six months.
In addition to a lactation space and pumping breaks, Dinour says companies that want to help their employees breastfeed should consider offering a third form of support, like flexible scheduling, making available a lactation consultant, or even offering on-site childcare.
Seemingly small things—like having to call a number to ask for a code for the lactation room when every other facility is accessed with a keycard, being told to ask your professor to use his office to express milk, or having to reach out to HR to navigate the return from maternity leave, instead of getting the information in “a beautifully formatted, carefully written email, like I get about everything else,” as one working mother remarked—can hurt when they seem like signs that the company you work for, and spend so much time thinking about, isn’t thinking about you at all. Simply knowing that your company is paying attention can make some less-than-perfect circumstances bearable. This is not to imply that accommodations don’t matter, but only that context matters, too.
When Rachel White gave birth to her second child, a daughter, in 2016, she had just finished her graduate degree and was preparing to begin a job teaching writing at Kansas City Kansas Community College. Her daughter was born in May, and the summer break served as a kind of unpaid maternity leave before she started the new job in August. “My supervisor was a father of two, and he was very upfront with me about wanting to balance his own family life and professional life,” says White. “He was very supportive, and showed me a room where I could pump, with a sign on the door that said ‘Lactation Room,’ and a lock, and that was amazing! I could use that between teaching classes.”
White, who described her time working at the community college as “an unbelievably positive experience,” ended up breastfeeding her daughter for nearly two years.

From: Harper's BAZAAR US
Source: Read Full Article
